Norwich hospital in Europe-wide trial using plant ingredients to counter risk of seizures and brain injury
A newborn boy who was delivered by emergency caesarean section in March at a Norwich hospital became the first baby in the world to join a cannabis-derived treatment trial.
The study is the first step in what researchers say could one day lead to a cannabis-derived medicine being used routinely in neonatal care to help babies at risk of seizures and brain injury.
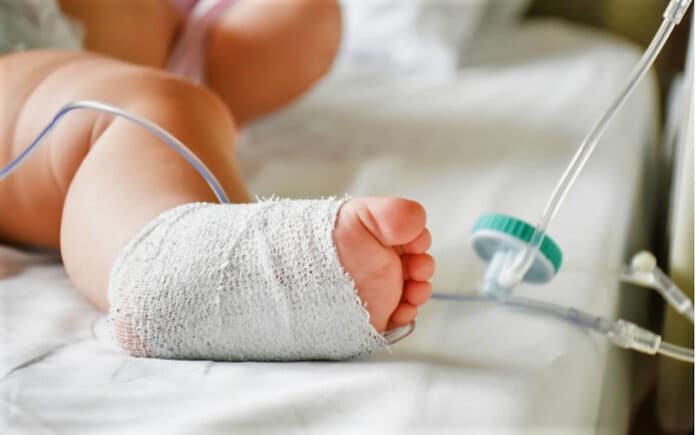
The baby, Oscar Parodi, was delivered on 11 March at Norfolk and Norwich university hospital (NNUH). He was unexpectedly born in a poor condition and needed to be transferred to the neonatal intensive care unit, where he had cooling therapy for 72 hours.
His mother, Chelsea Parodi, from Watton, Norfolk, said: “I was approached after the birth about taking part in this study and I consulted my mum and my brother who is training to be a paramedic. It was hard but I wanted to do everything I could to help my baby boy. Oscar was in hospital for nine days and he was being monitored 24/7.” Parodi said her son was “doing fantastically well”.
The study is examining whether the medicine is safe and effective in lessening the degree of brain injury for babies with the condition neonatal hypoxic ischemic encephalopathy (HIE).
Prof Paul Clarke, a consultant neonatologist at NNUH, said there was a lot of excitement at the neonatal intensive care unit. “This is the first time a cannabis-derived medicine has been tested intravenously in human babies. It is hoped that it will be good for preventing seizures and protecting the brains of newborn babies with HIE.
“We have always had good support from families wanting to take part in research on our [unit] and they often do it from an altruistic point of view to help benefit future babies. One of the attractions of this trial for parents is the closer brain monitoring babies get as part of the study, because a more advanced brainwave monitor is used for the trial babies. This gives parents more reassurance that any seizures will be picked up.”
A second child, born in April at the hospital, is also part of the trial. Children in the trial receive standard hypothermia treatment for HIE, where the whole body is cooled down to 33.5C, as well as a single dose of the study drug or placebo, followed by some tests to measure levels of the drug in the blood.
The trial, in which the drug is administered intravenously and in which the first babies to take part only receive a 30th of the usual dose, involves other neonatal intensive care units in the UK and elsewhere in Europe and will take a year to complete.
Babies in the trial will be given a single dose of study medication, or a placebo, as soon as possible within 12 hours of birth.
The therapeutic ingredient of the medicine occurs naturally in the cannabis plant and is extracted under highly controlled conditions to ensure that the tetrahydrocannabinol (THC) component which causes a “high” is minimal.
Clarke added: “As with any study of a new medicine there may be unexpected side effects and unknown risks. With this in mind the trial has been carefully designed to make it as safe as possible, and so we are only giving the babies a minuscule dose at the beginning, and we monitor them even more closely than usual.”